In humans, plants, and animals, infectious agents can spread from individual to individual, causing sickness. Even bacteria are not immune from infection; small viruses called bacteriophage seek out and attack bacteria, infecting them and using the bacterial cell machinery to create more copies of the bacteria. Today, we are obviously hearing about disease spread in the news with the COVID-19 Pandemic, but other infections like influenza, chicken pox, and the measles are still problematic. So, in this post, we’re going to talk about types of pathogens, how they spread, and how we can use testing (and a little bit of detective work) to determine the source of an infection.
So, first, I want to start with a few important terms. The first three – outbreak, epidemic, and pandemic – all relate to the spread of disease within an area. They differ in the scale. An outbreak is typically the smallest of the three. It refers to an increase in the incidence of cases of a specific disease in an area that is in excess of the normal number of cases in an area. For example, this could be the occurrence of Norovirus, a stomach virus, on a cruise ship. The virus may affect a large percentage of the population on the cruise ship, but it’s restricted to that place and time. An epidemic is one step larger: the pathogen is going to affect a larger number of people in a larger region. For example, due to a decrease in vaccination rates, the virus measles spread through Samoa, affecting a significant percentage of the population. A mass vaccination effort was able to slow the spread of disease, but not before nearly 6000 people got sick, and 83 children died. Today, we find ourselves in the midst of a pandemic – that is the outbreak of disease in many different geographic regions, affecting a substantial number of people. And the thing to remember about all of these definitions is that the numbers are relative. For example, seasonal flu vs pandemic flu. Every year, in the fall and winter there is a level of seasonal illness caused by the influenza virus, and this is something to be expected as people move indoors in cold weather. But when we start to see the number of cases of flu increase over what is expected based on historical data, researchers start to examine the virus more closely. And this is what happened in 2009, when a new strain of H1N1 swine flu emerged. The virus spread more quickly within the population, and caused more severe illness because there was no immunity to the virus within the community.
Now, in order to interrupt the spread of disease, public health professions will identify and contact any individuals which may have been exposed to the pathogen. In addition to allowing researchers to study the distribution patterns of the disease spread, it allows clinicians to provide treatment and counseling to exposed people, to notify possibly infected people so that they do not spread the disease further, and, of course, stop the spread of disease within a community.
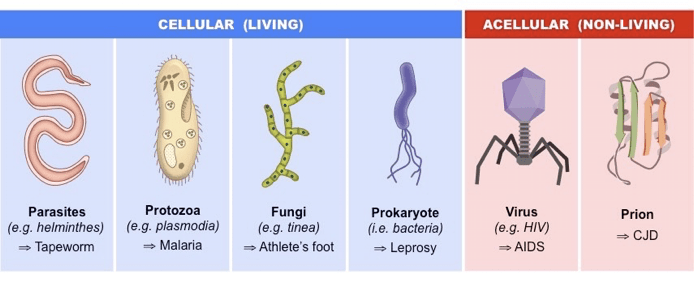
Infectious disease outbreaks are caused by pathogens, which in the broadest sense is any organism that can cause disease. This includes viruses, bacteria, fungi, and even proteins called prions that cause proteins to fold in the wrong way, which affects the nervous system. And many of these exist in and on your body at any given time, but when conditions change, they can invade the body and cause disease.
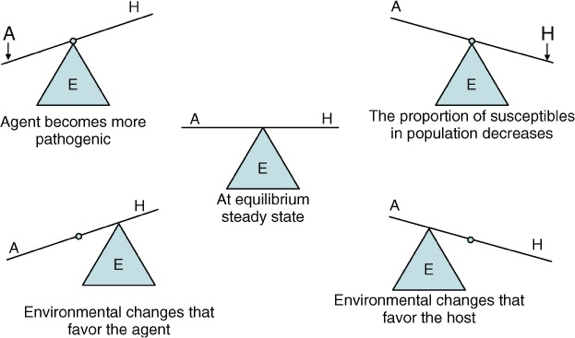
There are many models for the spread of disease, but one of the most common is the epidemiology triangle, where the host, the infectious agent, and the environment are all in balance with one another. And this would be considered the normal state. In this model, the host is an organism that is susceptible to an infectious agent. The environment brings the host and the agent together. And these three conditions interact with one another.
A long as they are in balance, there’s no problem, and we see that in the graphic in the middle of this slide. But, when the balance tips, the host can become sick. And there are examples of how that balance can shift on this slide. So if a virus becomes more pathogenic, the scale is tipped in favor of the agent and the individual gets sick. If the numbers of a pathogen changes, that can affect the host – so 10 virus particles might not cause sickness, but 1000 does. Or, with a vaccine, the number of hosts decrease so fewer people are infected. Or, the environment can change to influence the host-agent interaction. For example, we see cough and cold more often in the fall and winter, when we move indoors because of the cold weather. To best control the spread of disease, all three of these factors must be considered.
There are many ways that disease can spread between people. Pathogens can be spread through abiotic, or physical means. This could be wind spreading fungi spores, or the entry of parasites into the bloodstream through cuts in the skin. Animals are also vectors for disease – that is, any agent that carries and transmits a pathogen between organisms. And one common vector is the mosquito, which can transmit malaria, yellow fever, and zika virus.
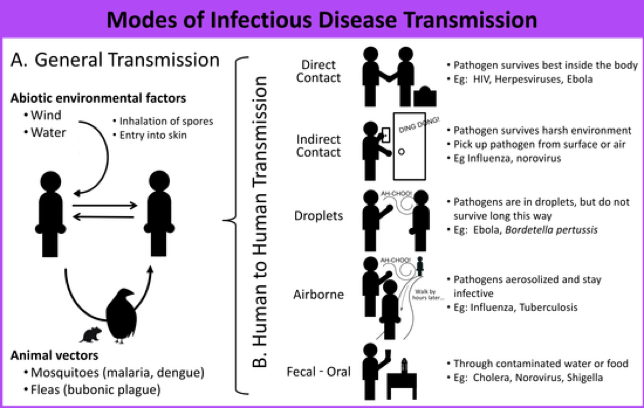
Diseases are also transmitted directly between people in human to human transmission. That can be through direct contact with blood or body fluids from infected people, that’d be like the Ebola virus which is transmitted through blood. These viruses are generally easy to kill, and do not last long when not in their preferred environment.
Indirect contact happens when an infectious agent can survive in harsh events and you can pick them up from contaminated surfaces. And you might hear about people talk about fomite transmission, and that refers to transmission from objects that are likely to carry the infection like doorknobs, or clothing, or even the ever-present cell phone. And so this is what happens with viruses like the flu, or norovirus.
Droplet and airborne transmission both refer to liquid droplets from the mouth that happen when we cough or sneeze. The largest particles, droplets, don’t last long because they can’t remain in the air. However, smaller droplets, suspended in the air as aerosols, can travel through a further distance and infect people. And so this is a common mode of transmission for respiratory viruses.
And finally, there is the fecal-oral route, where pathogens in human waste enter the food or water supply though contaminated water, or poor hand-washing after using the bathroom. A common pathogen spread this way is Cholera. While modern sanitation and water treatment has eliminated Cholera in industrialized areas, it still affects millions of people per year.
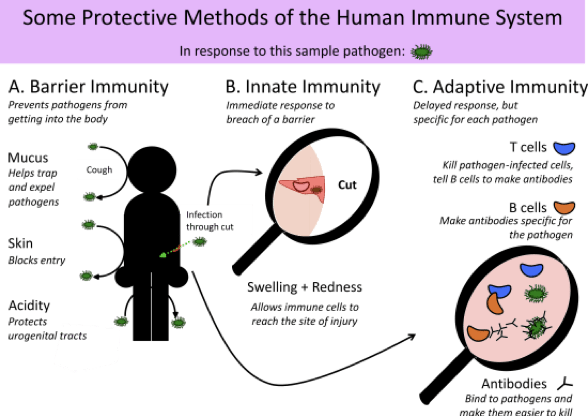
Luckily, the human body has several methods to protect us from disease, or else we’d always be sick! First, there are physical barriers that prevent pathogens from getting into our bodies. This includes skin barrier, which is largely impermeable. It keeps water and body fluids in, and bacteria and other pathogens out. We have mucus in our sinuses which traps microorganisms, and moves them out of the body. Further more, we have areas of the body with pHs that are largely inhospitable to microbes, like the highly acidic environment of the stomach.
If a pathogen gets into the body, the human immune system fights them off. The first is the innate immunity, where immune cells reach the site of the break in the skin to neutralize the pathogen. And this is a general interaction, where any pathogen would be attacked and treated. The second is adaptive immunity, where the immune system creates a response that targets specific pathogens. In the first infection, the body creates antibodies that target and neutralize the pathogens. After the infection, the body remembers the pathogen. If the pathogen enters the body again, the antibodies already exist and the body can attack it more quickly. In many cases, the host won’t get sick at all, or the symptoms would be mild.
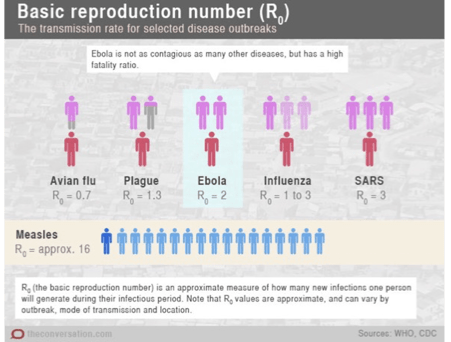
Researchers evaluate the spread of disease using the R-naught, which is an average of how many people will contract a pathogen from one infected person during their infectious period. There are many variables that factor into this number, but the three most important are the number of people the infected person contacts, the likelihood of infecting that secondary contact, and the infectious period. So, if one person had contact with three people per day, and had a 1 in 3 chance of being infected, and the infectious period was three days, we’d have an R-naught of 3.
In general, a r-naught above 1 means that the virus is able to quickly spread through a community unchecked, and the number of people will increase exponentially. An r-naught below 1 means that the spread of the virus is slowing and can likely be contained. Now, these can change over time. The numbers here are averages based on data from past outbreaks. For current transmission, like that with COVID-19, which is a new disease, it’s a lot harder. The r-naught is constantly changing, and it can be different between communities. There’s no historical data. But it can help scientists, doctors, and public health professionals make recommendations for policies to contain the disease locally and regionally.
Luckily, with proper precautions, we can prevent the spread of disease. Airborne pathogens like COVID-19 or Influenza spread person-to-person through liquid droplets that come out when you cough or sneeze, so this is why we need to be careful to sneeze into a shoulder or a tissue. Furthermore, we can wear cloth masks to cover the mouth and nose, which prevent our respiratory droplets from spreading via cough or sneeze. Right now, while a disease is spreading, we can take actions like social distancing to reduce the likelihood of infecting those around us, which can the spread of the disease.

Gastrointestinal disease can spread through contaminated food or infected surfaces, but foodborne illnesses can be prevented. Use proper food storage and handling techniques to prevent illness.
Touching your face with contaminated hands can introduce the virus to your mucus membranes, so it is important to keep hands away from your eyes, nose and mouth. Luckily, soap, hand sanitizer and other disinfectants kill many pathogens, so frequent washing of hands can limit its spread.
If you are exhibiting serious symptoms, contact your healthcare professional for guidance. The most important thing is that if you are exhibiting symptoms of a serious illness, please reach out to your doctor or your local public health officials. There is a lot of information on the internet about the COVID-19 pandemic on the internet, some of which is intentionally misleading. The best source of information will come from the Centers for Disease Control and Prevention (CDC) or the World Health Organization.
Do you want to learn how to model the spread of disease in your classroom? We describe how you can use Edvotek Kit S-68, What is an Epidemic and How Does An Infection Spread? in a previous live stream, available on YouTube. The slides are downloadable as well to help with your pre-lab preparation.



1 comment
Comments are closed.