Antibiotic resistance is one of the world’s most urgent public health problems. In 2019 an estimated 4.95 million people died from illnesses involving antibiotic-resistant bacteria and fungi. (In comparison that year 1.51 million individuals died from malaria and HIV/AIDS.) Resistance occurs when bacteria develop the ability to defeat the drugs designed to kill them. This is happening at an accelerated and concerning rate due to the increased use – and misuse – of antibiotics.
Addressing the growing threat of antibiotic resistance requires global action by researchers, healthcare professionals, policymakers, and the public. A good first step? Knowing the enemy. Read on to find out about three of the most feared antibiotic-resistant bacteria, no PPE required!
Staphyloccocus aureus
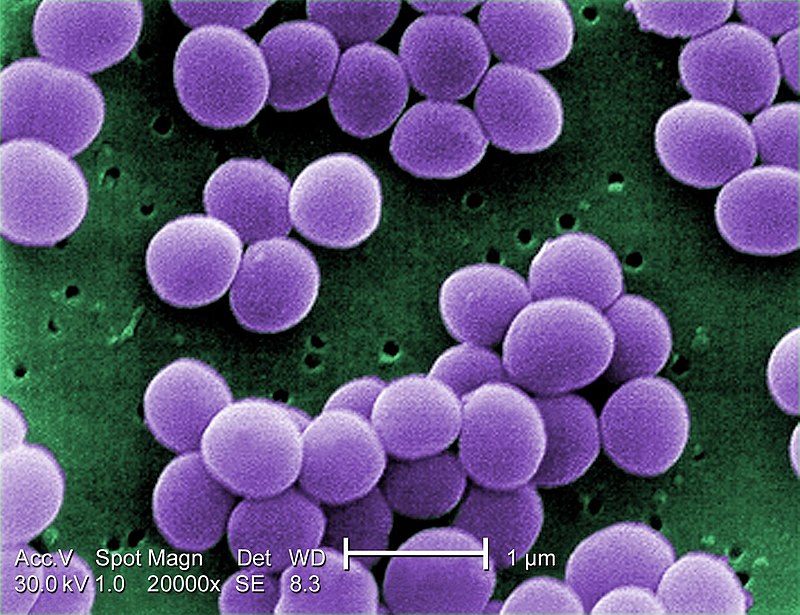
This gram-positive bacteria is an opportunistic pathogen. This means that under normal conditions it’s benign. In fact, S. aureus is found on the skin and in the upper respiratory tract of nearly a third of humans. However, things can quickly take a turn for the worse when the bacteria infect an immunocompromised host. In such individuals, S. aureus or ‘staph’ can cause dangerous conditions like meningitis, pneumonia, osteomyelitis (bone infections), toxic shock syndrome, sepsis, and heart failure. The untreated case fatality rate of these infections is 80%, while the treated case fatality rate is 15-50% depending on the health and age of the patient and the antibiotic resistance of the strain. Unfortunately, S. aureus is notorious for its ability to become resistant to antibiotics. Today 95.2% of the species is highly resistant to penicillin and 84.6% to cephalexin – two of the most popular antibiotics. Even more concerning are the strains that can survive “top-shelf” antibiotics. These include vancomycin-resistant S. aureus (VRSA), vancomycin-intermediate S. aureus (VISA), methicillin-susceptible S. aureus (MSSA), and of course methicillin-resistant S. aureus (MRSA).
Klebsiella pneumoniae
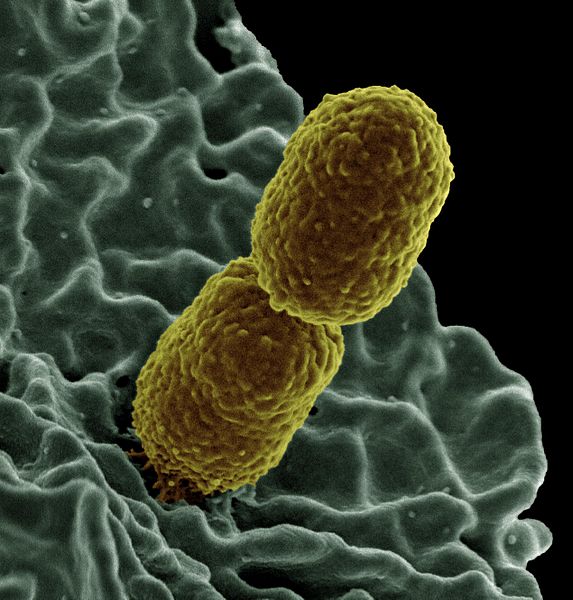
This gram-negative bacteria is another opportunistic pathogen that causes a range of diseases including pneumonia, blood clots, urinary tract infections, wound and surgical infections, sepsis, and meningitis. Even more concerning is the discovery of a new variant called hypervirulent K. pneumonia or hvKP which causes disease in even healthy individuals and infects almost all parts of the body including the eyes and central nervous system. Almost all K. pneumonia contain a beta-lactamase gene that gives them resistance to ampicillin and ampicillin-related antibiotics. The species is also adept at using and sharing plasmids – genetic structures in bacteria cells that replicated independently of the chromosomes. As a result, many variants are also resistant to additional antibiotics such as carbapenem and even the “last resort” antibiotic colistin.
Acinetobacter baumannii
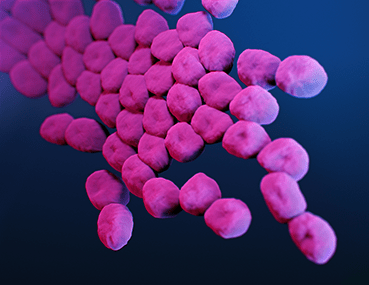
This gram-negative bacteria is a leading cause of nosocomial (hospital-derived) infection. It’s often called Iraqibacter because it was first found in several military treatment facilities during the Iraq war and continues to be an issue for soliders and veterans. Infections by A. baumannii can cause fever, confusion, pain urinating, sensitivity to light, nausea, chest pain, cough, and necrosis near wounds and/or surgical sites. The species shows an impressive level of genetic flexibility thanks to its ability to integrate foreign DNA, rearrange its genome, and rapidly mutate. Consequently, many variants have developed resistance to several types of antibiotics. Luckily scientists have had some success treating antibiotic resistance A. baumannii infections with phage therapy (using viruses to kill or weaken bacteria).
November 18-24 is World Antimicrobial Awareness Week. Bring this pressing global health issue safely into your classroom with these resources, lesson plans, and experiments!
1. PBS Classroom Activity: Killer Microbe
2. ReAct Educators Toolbox
3. Edvotek Experiment: Identification and Characterization of Bacteria
4. Edvotek Experiment: Testing the Effectiveness of Antibacterial Cleaners


2 comments
Comments are closed.